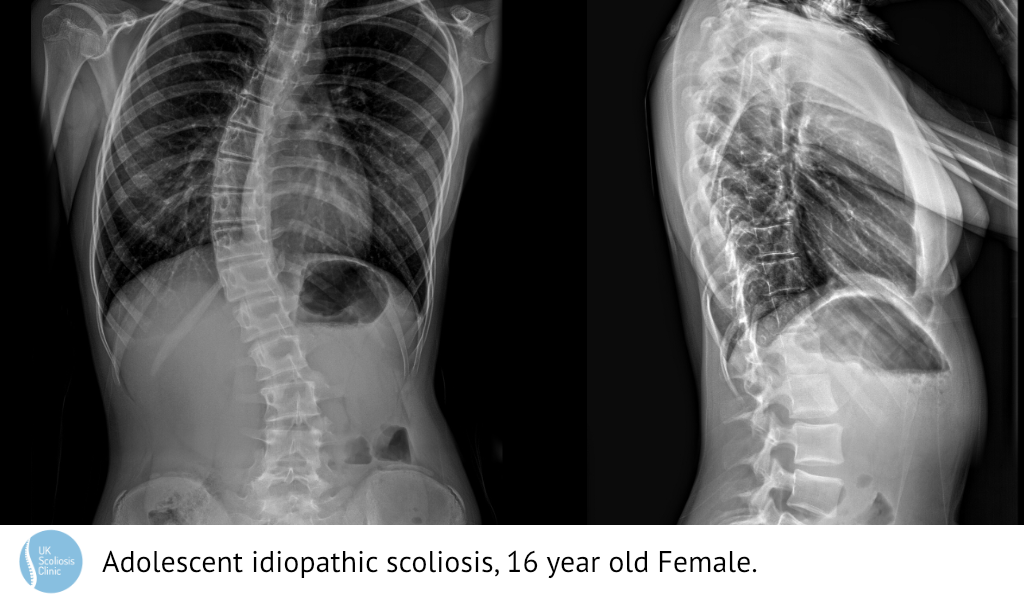
Most of the Scoliosis cases we treat at the clinic – and indeed, most of the scoliosis cases discovered are categorised as adolescent idiopathic scoliosis (often called AIS) That’s to say, scoliosis in a person older than 10, but who has not yet reached skeletal maturity, and a case without obvious cause, such as congenital or syndromic issues, or trauma.
Whereas infantile and younger Juvenile scoliosis cases are common in boys, 80% of all AIS cases are girls. It is usually noticed around 11-12 years of age in girls and slightly later when diagnosed in boys. AIS is estimated to affect between 3 and 4% of teenagers. In most cases, AIS begins to develop noticeably at the initial onset of puberty and becomes more apparent as it worsens during growth spurts. AIS can be highly progressive, so it is important that the right sort of monitoring and treatment is sought as soon as the condition is noticed. When not appropriately treated it may result in significant deformity, physical disability and psychological issues – but when treated with effective modern approaches, the prognosis – as showed by the BrAIST study, is good – with as many as 90% of patients who comply with bracing prescriptions avoiding surgery[1]
What causes AIS?
Like all forms of idiopathic scoliosis, the exact cause of AIS is unknown. Like other forms, there have been a large number of possible causes suggested – one of the leading theories is a genetic link, although more research is required before we are able to make a definitive conclusion.
There is also some evidence that AIS may be associated with certain activities which stress and pull the spine away from its normal aligned position – for example, research indicates a higher incidence of scoliosis in ballet dancers and gymnasts, although it’s important to note that this does not necessarily mean that these activities cause Scoliosis, only that more cases are being detected (this could feasibly be simply because we’re looking for them more frequently).
It’s also worth clarifying that while scoliosis does cause postural issues, poor posture does not cause scoliosis, and nor (so far as the current research suggests) does diet.
What is the prognosis for AIS Scoliosis?
The prognosis for an AIS case depends on a number of key factors – the significance of the curve at the time of discovery, the flexibility of the curve, the age of the patient and the ability of the patient to comply with ongoing treatment.
The larger a curve is at discovery, the more work needs to be done to correct it – Bracing has been shown to be effective up to 60 degrees, but an ideal candidate is in the 20-40 degree range. Closely tied to this is the rigidity of the curve – that is to say how flexible the spine is, and therefore how likely we are to succeed with an approach such as bracing, which aims to gently guide the spine back to a correct alignment. A flexible curve is much easier to treat than a rigid one.
The age of the patient is important for two reasons – firstly, while scoliosis development does not always stop in adults, where it does continue it tends to slow and become predictable – developing at about 1 degree per year. Therefore a small curve in an individual close to adulthood has less time to progress to a significant degree, than does a large curve in a younger child. What’s more, research suggests that curves that are still small at adulthood do not continue to develop[2]
Secondly, it’s also long been thought that scoliosis worsens faster around growth spurts[3] – hence an older adolescent who has almost reached their full growth has less exposure to this potentially aggravating factor. More recently, however, we have come to understand aspects such as the Risser sign (an indication of skeletal maturity) and the onset of menstruation are closely correlated with the potential for curve increase regardless of “growth spurts”. Immature children (Risser sign 0 or 1) with larger curves (20–29°) at initial diagnosis demonstrated a 68% risk for curve progression, whereas mature children (Risser 2–4) with similar curves at initial presentation had a 23% risk for curve progression. Conversely, immature children with smaller curves (5–19°) demonstrated 22% chance for curve progression, while mature children with smaller curves had only a 1.6% risk for curve progression.[4]
In both cases, we would like to detect and control curves in patients at the earliest possible opportunity, as this allows us to stabilise curves, and prevent progression throughout growth, and maximise the chance for curve correction and the avoidance of future issues in adulthood.
It’s for this reason that early screening and detection is so important in scoliosis cases – it’s too simplistic to say that cases that are detected early are guaranteed a better outcome, but by spotting cases as early as possible, you certainly allow the maximum number of options for treatment.
How can we treat AIS?
The best treatment for a scoliosis case depends on all of the above factors – but for simplicity, let’s take the question just by curve size. It’s important to remember that factors such as age and curve flexibility may modify this rough outline.
In curves between 10-20° scoliosis, specific exercises – a physiotherapy based approach to treatment – are typically recommended as an initial approach, while bracing may also be used as a preventative measure in the long term, or as a more convenient alternative to exercise-based approaches.
In curves over 20-25° with a moderate to high risk of progression, scoliosis bracing is typically considered and often will be used in conjunction with scoliosis specific exercise. As we discussed a the beginning of the month – bracing was shown to be effective in reducing the progression to the surgical threshold of 50° by the end of growth in 72% of cases compared to 48% of those who were purely observed. What is important to remember, is that those who wore the brace for more than 13 hours per day actually had a 90% success rate[5].
In curves 45-50°, conservative non-surgical treatment becomes more difficult. In older adolescents when a curve is less likely to rapidly progress, bracing may be used and combined with intensive scoliosis specific exercise. This may help to improve body aesthetics and reduce the curve size when surgery is not recommended.
In large curves in younger adolescents with a high risk of progression, or a high rate of curve development bracing may be used to slow curve development. This way surgery can be delayed until growth has finished so multiple surgeries are not required.
When curves are large and the risk of progression is high, surgery may be the only option. Surgery is recommended not purely on curve size, but also on curve location, future progression, loss of postural balance and when bracing has been unsuccessful.
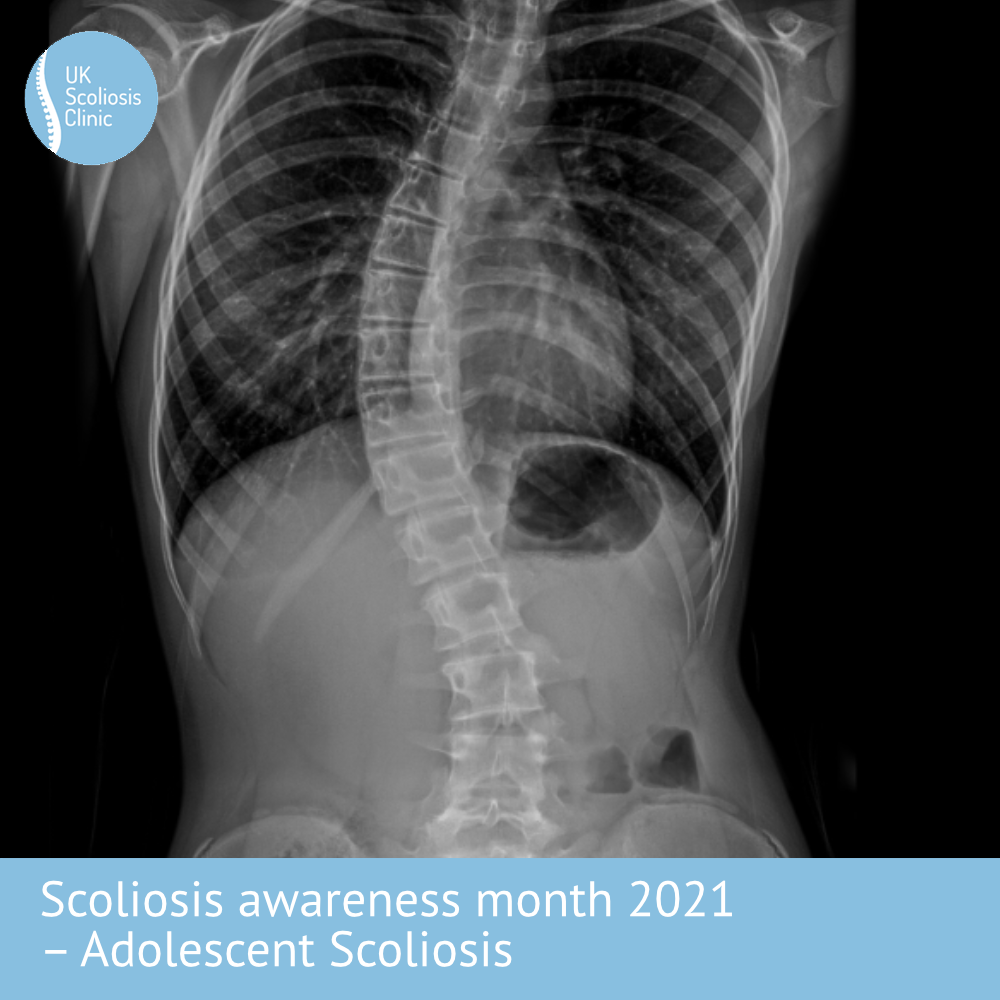
What does Adolescent Scoliosis look like?
The below X-ray shows an example AIS case. It’s usually not possible to tell how severe scoliosis is without taking an X-ray, although external signs can suggest that the condition may be present. This is why regular screening is so important!
[1] Stuart L. Weinstein, M.D., Lori A. Dolan, Ph.D., James G. Wright, M.D., M.P.H., and Matthew B. Dobbs, M.D. Effects of Bracing in Adolescents with Idiopathic Scoliosis, N Engl J Med 2013; 369:1512-1521
[2] Weinstein SL, Ponseti IV: Curve progression in idiopathic scoliosis. J Bone Joint Surg (Am) 1983, 65:447-455.
Weinstein SL, Zavala DC, Ponseti IV: Idiopathic scoliosis: longterm follow-up and prognosis in untreated patients. J Bone Joint Surg (Am) 1981, 63:702-712.
Ascani E, Bartolozzi P, Logroscino CA, Marchetti PG, Ponte A, Savini R, Travaglini F, Binazzi R, Di Silvestre M: Natural history of untreated idiopathic scoliosis after skeletal maturity. Spine 1986, 11:784-789.
[3] Duval-Beaupere G: Pathogenic relationship between scoliosis and growth. In Scoliosis and Growth Edited by: Zorab P. Edinburgh, Scotland: Churchill Livingstone; 1971:58-64.
[4] Bunnell WP: The natural history of idiopathic scoliosis before skeletal maturity. Spine 1986, 11:773-776.
[5] Stuart L. Weinstein, M.D., Lori A. Dolan, Ph.D., James G. Wright, M.D., M.P.H., and Matthew B. Dobbs, M.D. Effects of Bracing in Adolescents with Idiopathic Scoliosis, N Engl J Med 2013; 369:1512-1521